CBS News Live
CBS News Baltimore: Local News, Weather & More
Watch CBS News

Key Bridge salvage crews Thursday are pre-rigging a large portion of steel from the collapsed bridge before it is moved to nearby Sparrows Point.

A Montgomery County high school student is facing charges after allegedly planning to commit a school shooting, according to police.

Governor Wes Moore announced the start of the Port of Baltimore Worker Support Program Friday, which will provide temporary cash assistance to eligible workers who have lost income and work hours due to the Francis Scott Key Bridge collapse.
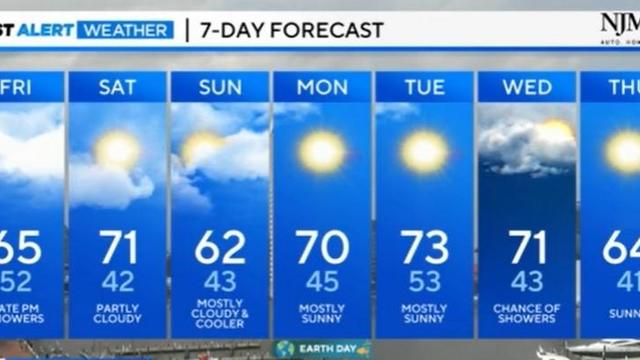
Nice weather returns for your outdoor weekend plans

An 18-year-old Montgomery County teen was denied bond at a court hearing today, after he was charged with what police describe as plans to commit a school shooting at a high school.

Leaders from the Small Business Association traveled to Baltimore to talk about the federal resources available to businesses impacted by the Key Bridge collapse.

Crews continue to work 24/7 on salvage operations related to the Francis Scott Key Bridge collapse, Gov. Wes Moore and other leaders made it clear Friday it's still full steam ahead.

Marie Barton is emotional and shocked that Nick's Law passed both chambers unanimously. Now it needs the signature from Governor Wes Moore.

A disappearing lizard population in the mountains of Arizona shows how climate change is fast-tracking the rate of extinction.

Scattered showers moving through the region this afternoon will move out by sunset. Skies will remain mostly cloudy with temps in the 60s.

Governor Wes Moore announced the start of the Port of Baltimore Worker Support Program Friday, which will provide temporary cash assistance to eligible workers who have lost income and work hours due to the Francis Scott Key Bridge collapse.

Leaders from the Small Business Association traveled to Baltimore to talk about the federal resources available to businesses impacted by the Key Bridge collapse.

Key Bridge salvage crews worked to rig a large portion of steel from the collapsed bridge Thursday before it is moved to nearby Sparrows Point.

It was clear from the start of this offseason that the Baltimore Ravens were going to lose quite a few players to free agency.

Baltimore Ravens wide receiver Zay Flowers was cleared by the NFL after an investigation into violation of the personal conduct policy.

Former Baltimore Ravens' second-round draft pick J.K. Dobbins is reportedly signing with the Los Angeles Chargers.

The Orioles (12-6), winners of four in a row, defeated the Twins, 4-2.

Orioles pitcher Grayson Rodriguez allowed two runs on four base hits in six innings.

The program operates through a series of anywhere from 4-6 workshops that each focus on a particular aspect of learning and development, and how parenting practices that incorporate purposeful play can support each particular domain.
Falsettos is about neurotic New Yorker Marvin, who leaves his wife Trina & son Jason for his lover Whizzer
Renowned Gospel artist Donald Lawrence is set to take that 2024 GospelFest at the Joseph Meyerhoff Symphony Hall, led by conductor Dr. Henry Panion III on April 27

City Ranch says its lessons are designed to be educational and engaging for people from all walks of life.
All of the proceeds from wellness day at Four Seasons will benefit Camp B'more, a weeklong urban summer camp

The event supports the medical center's sexual assault and domestic violence program, which provides confidential services to victims of all ages, at no cost to the patient.
Champ is a Yorkshire Terrier found as a stray dog in Towson, Maryland

The steakhouse is located at MGM National Harbor Resort and Casino

The Maryland Chapter of the Cystic Fibrosis Foundation will host the 8th Annual "Feastival, A Food Adventure for a Cure" on April 13, 2024 from 1 to 4 pm at the Inner Harbor’s West Shore Park.

An 18-year-old Montgomery County teen was denied bond at a court hearing today, after he was charged with what police describe as plans to commit a school shooting at a high school.

Crews continue to work 24/7 on salvage operations related to the Francis Scott Key Bridge collapse, Gov. Wes Moore and other leaders made it clear Friday it's still full steam ahead.

Here's your Friday evening news round up | 04/19/2024

Scattered showers moving through the region this afternoon will move out by sunset. Skies will remain mostly cloudy with temps in the 60s.

Leaders from the Small Business Association traveled to Baltimore to talk about the federal resources available to businesses impacted by the Key Bridge collapse. But not all business owners have been able to receive the help they need.

Key Bridge salvage crews Thursday are pre-rigging a large portion of steel from the collapsed bridge before it is moved to nearby Sparrows Point.

A Montgomery County high school student is facing charges after allegedly planning to commit a school shooting, according to police.

Governor Wes Moore announced the start of the Port of Baltimore Worker Support Program Friday, which will provide temporary cash assistance to eligible workers who have lost income and work hours due to the Francis Scott Key Bridge collapse.

Nice weather returns for your outdoor weekend plans

An 18-year-old Montgomery County teen was denied bond at a court hearing today, after he was charged with what police describe as plans to commit a school shooting at a high school.

Marie Barton is emotional and shocked that Nick's Law passed both chambers unanimously. Now it needs the signature from Governor Wes Moore.

Key Bridge salvage crews worked to rig a large portion of steel from the collapsed bridge Thursday before it is moved to nearby Sparrows Point.

As salvage operations continue at the Francis Scott Key Bridge collapse site, the owners of the Dali have invoked a centuries-old maritime law requiring cargo owners to contribute to the costs of salvaging the ship and its cargo.

It is certainly a seller's market right now, but if you're looking to buy a home in Maryland you won't want to wait around too long.

Kenneth Davis, 32, allegedly shot and killed 25-year-old Tracey Elizabeth Carrington as she was leaving a Baltimore bar.

The program operates through a series of anywhere from 4-6 workshops that each focus on a particular aspect of learning and development, and how parenting practices that incorporate purposeful play can support each particular domain.
Falsettos is about neurotic New Yorker Marvin, who leaves his wife Trina & son Jason for his lover Whizzer

Renowned Gospel artist Donald Lawrence is set to take that 2024 GospelFest at the Joseph Meyerhoff Symphony Hall, led by conductor Dr. Henry Panion III on April 27

City Ranch says its lessons are designed to be educational and engaging for people from all walks of life.

All of the proceeds from wellness day at Four Seasons will benefit Camp B'more, a weeklong urban summer camp

It was clear from the start of this offseason that the Baltimore Ravens were going to lose quite a few players to free agency.

Baltimore Ravens wide receiver Zay Flowers was cleared by the NFL after an investigation into violation of the personal conduct policy.

Former Baltimore Ravens' second-round draft pick J.K. Dobbins is reportedly signing with the Los Angeles Chargers.

The Orioles (12-6), winners of four in a row, defeated the Twins, 4-2.

Orioles pitcher Grayson Rodriguez allowed two runs on four base hits in six innings.

The Supreme Court will consider Monday whether bans on public camping constitute "cruel and unusual punishment" barred by the Eighth Amendment.

Hogan hopes to become the first Republican in more than 40 years to win a Senate seat in deep-blue Maryland, where Democrats outnumber Republicans 2-1 statewide.

The Supreme Court seemed divided over a case challenging the scope of a federal obstruction law that prosecutors have used to charge more than 300 Jan. 6 defendants.

The investigation is being conducted by Maryland's U.S. Attorney's Office and the FBI.

The White House is turning to other methods to erase student debt after the Supreme Court blocked its broader effort to forgive loans.

When it comes to vintage style, art and innovation—Baltimore is home to it all.

The University of Maryland Medical Center was granted the American Nurses Credentialing Center's (ANCC) Magnet for the fourth time in a row.

Magali Uroza comes from a Mexican immigrant family and remembers the challenges of learning English while growing up in Baltimore.

It is the cherry trees' second-earliest peak bloom on record and follows one of Washington's warmest recorded winters. In 1990, the trees blossomed on March 15.
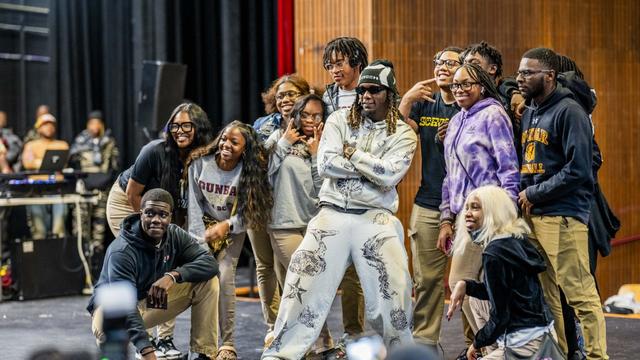
Georgia rapper Offset surprised students at Dunbar High School on Tuesday for their stellar academic performance and attendance according to the Baltimore Police Department.

The Maryland Food Bank is on pace to distribute more than 52 million pounds of food, which is a 20 percent jump in comparison to pre-COVID times.

It has long been a popular resource in the community, easily accessible to many college students and neighbors.

Has mom and dad's bank been open too long at your house?

According to a report from the National Institute on Retirement Security, 40% of Gen Xers have zero dollars saved for retirement.

According to Bankrate, Baltimore is one of the top 10 most affordable cities for buying used cars.

Primanti Bros. on Tuesday announced plans to expand to the Baltimore region this spring.

CVS is closing dozens of pharmacies inside Target stores in 2024 as the store and other retail pharmacy chains face increasing difficulties.

The wildly popular chicken finger joint opened its doors Tuesday at the Snowden River Shopping Center.

The council passed the "Bring Your Own Bag Act" with a bipartisan vote in February.

Baltimore is one of 31 designees announced Monday, picked from nearly 400 applicants.

Health officials are warning consumers not to consume Infinite Herbs basil sold at some Trader Joe's and Dierberg's stores after 12 people were sickened.

Most worrisome gaps involve cancer chemotherapy drugs, ER medications and and therapies for ADHD.

The prepackaged boxes of deli meat, cheese and crackers are not a healthy choice for kids, advocacy group says.

The University of Maryland Medical Center was granted the American Nurses Credentialing Center's (ANCC) Magnet for the fourth time in a row.

The state aims to force the company to make necessary repairs and impose fines of up to $25,000 per violation.

The significance of the song was amplified by praise from music legend Paul McCartney, who called the recording "magnificent" and appreciated its reinforcement of the civil rights message he intended when writing "Blackbird."

Charli XCX and Troye Sivan are stopping in Baltimore this fall on a joint tour.

In the 1,000th episode, titled "A Thousand Yards," NCIS comes under attack by a mysterious enemy from the past.

A Billy Joel special on CBS and Paramount+ will air again after it was cut off in the middle of the singer's performance of "Piano Man."

The show, renowned for its thrilling investigations and dedicated team, has become a cornerstone of television drama.

Scattered showers moving through the region this afternoon will move out by sunset. Skies will remain mostly cloudy with temps in the 60s.

Dry weather returns this weekend!

Meteorologist Abigail Degler has your Friday morning forecast 4/19/2024

Derek Beasley has your Thursday night forecast (4/18/2024)

Derek Beasley has your Thursday evening forecast (4/18/2024)

An 18-year-old Montgomery County teen was denied bond at a court hearing today, after he was charged with what police describe as plans to commit a school shooting at a high school.

Crews continue to work 24/7 on salvage operations related to the Francis Scott Key Bridge collapse, Gov. Wes Moore and other leaders made it clear Friday it's still full steam ahead.

Here's your Friday evening news round up | 04/19/2024

Scattered showers moving through the region this afternoon will move out by sunset. Skies will remain mostly cloudy with temps in the 60s.

Leaders from the Small Business Association traveled to Baltimore to talk about the federal resources available to businesses impacted by the Key Bridge collapse. But not all business owners have been able to receive the help they need.